Diaphragm dysfunction (DD) frequently develops in critically ill patients and is associated with adverse outcome, including prolonged duration of mechanical ventilation and increased length of ICU stay.1,2 Risk factors for the development of diaphragm dysfunction include sepsis and mechanical ventilation. Both ventilator over-assist and ventilator under-assist are associated with development of respiratory muscle weakness. Therefore, monitoring diaphragm activity using non-invasive, reproducible methods may be of clinical importance.
Ultrasound of the diaphragm allows quantification of excursion, thickness and thickening fraction, which can be used to estimate diaphragm function. Diaphragm ultrasound is used to evaluate the anatomy and function of the diaphragm. It is a safe, repeatable, accurate, non-invasive bedside technique that can be successfully applied indifferent settings, including general intensive care and the emergency department.
Techniques & views
Diaphragm
Unilateral nerve damage affects only one hemidiaphragm and therefore, ultrasound evaluation of both sides is recommended, although the left hemidiaphragm may not be as easily visualized. Two ultrasound approaches to visualize the diaphragm can be performed: the midaxillary intercostal approach at the zone of apposition, and the subcostal approach using the liver or spleen as an acoustic window.
Intercostal approach: Thickness and Thickening Fraction
The intercostal approach is performed with a 10-15-MHz linear array transducer positioned in a cranio-caudal direction and perpendicular to the skin in the zone of apposition between the mid-axillary or antero-axillary line, in the 8th to 11th intercostal space. The diaphragm will usually appear at a depth of 2-4 centimeters as a three-layered structure between the pleural and peritoneal membrane (Figure 1). Characteristically, a white linear structure is seen in the middle of the diaphragm. We recommend to measure diaphragm thickness perpendicular to its fiber direction between the pleural and peritoneal membrane (Figure 1). The lower limit for normal diaphragm thickness is around 1.5 mm in healthy subjects.
As with any other skeletal muscle, the diaphragm thickens with active shortening and therefore, its thickening reflects contractile activity. Thickening fraction (TFdi) can be calculated in B-mode or M-mode as the percentage inspiratory increase in diaphragm thickness relative to end-expiratory thickness during tidal breathing (TFdi) or maximal inspiratory effort (TFdi(max)): TFdi = (end inspiratory thickness - end expiratory thickness) / end expiratory thickness *100%. (Figure 1). Inspiratory thickening of the diaphragm can be used to assess muscle function.
Subcostal approach: Excursion
Diaphragmatic excursion is the result of diaphragmatic muscular tone and transdiaphragmatic pressure. So, factors influencing transdiaphragmatic pressure generating capacity will also affect excursion. The relationship between transdiaphragmatic pressure and excursion is, however, confounded by respiratory mechanics and by mechanical ventilatory support.
Diaphragmatic excursion is measured with a low frequency phased-array or curved-array (“abdominal”) probe (2-5MHz) positioned just below the costal arch at the midclavicular line, with the patient in semi-seated position and by angling the ultrasound beam as much as possible cranially and perpendicular to the diaphragmatic dome (Figure 2). The diaphragm is identified as a bright line covering the liver and the spleen. Obtaining a clear image of the left hemidiaphragm can be difficult due to the poor acoustic window of the spleen. During inspiration, the diaphragm should move towards the probe (Figure 2). Excursion is quantified in M-mode, with the M-line placed perpendicular to the direction of motion (Figure 1); To acquire the best measurement, the sweep speed is adjusted to around 10 mm/s to obtain a minimum of three respiratory cycles within one image. Diaphragm excursion should only be measured during unassisted breathing , since active contraction of the diaphragm cannot be distinguished from passive displacement due to ventilator inspiratory pressures.
In a cooperative patient, a maximum inspiratory effort is performed to assess maximal excursion. Excursion of both hemidiaphragms is compared to identify unilateral weakness or paralysis. The success rate for visualizing excursion is high during tidal breathing.
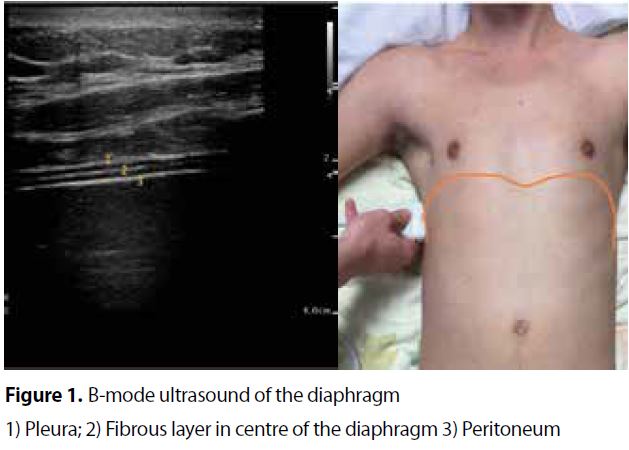
Adapted from ref 2
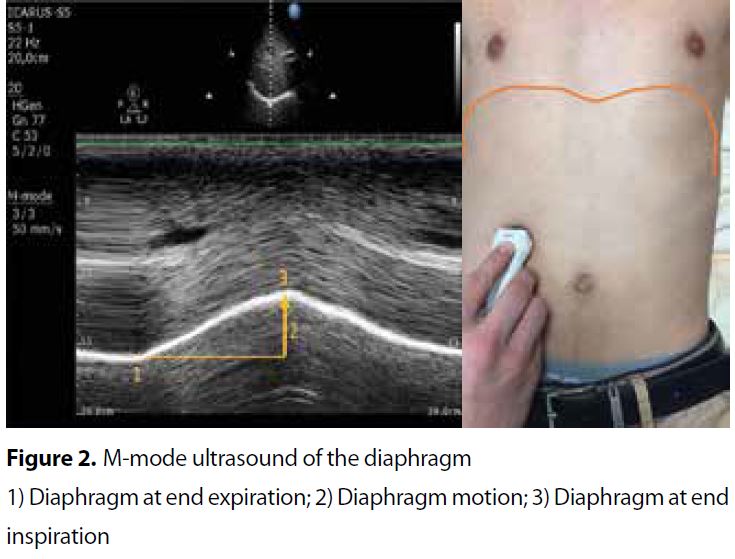
Diaphragm excursion, also called diaphragm motion; Adapted from ref 2
references:
- Tuinman PR, Jonkman AH, Dres M, Shi ZH, Goligher EC, Goffi A, de Korte C, Demoule A, Heunks L. Respiratory muscle ultrasonography: methodology, basic and advanced principles and clinical applications in ICU and ED patients-a narrative review Intensive Care Med. 2020 Jan 14
- M.E. Haaksma, L. Atmowihardjo, L. Heunks, A. Spoelstra-de Man, P.R. Tuinman. Ultrasound imaging of the diaphragm: facts and future. A guide for the bedside clinician. Neth J Crit Care March 2018;26(2): 58 - 63
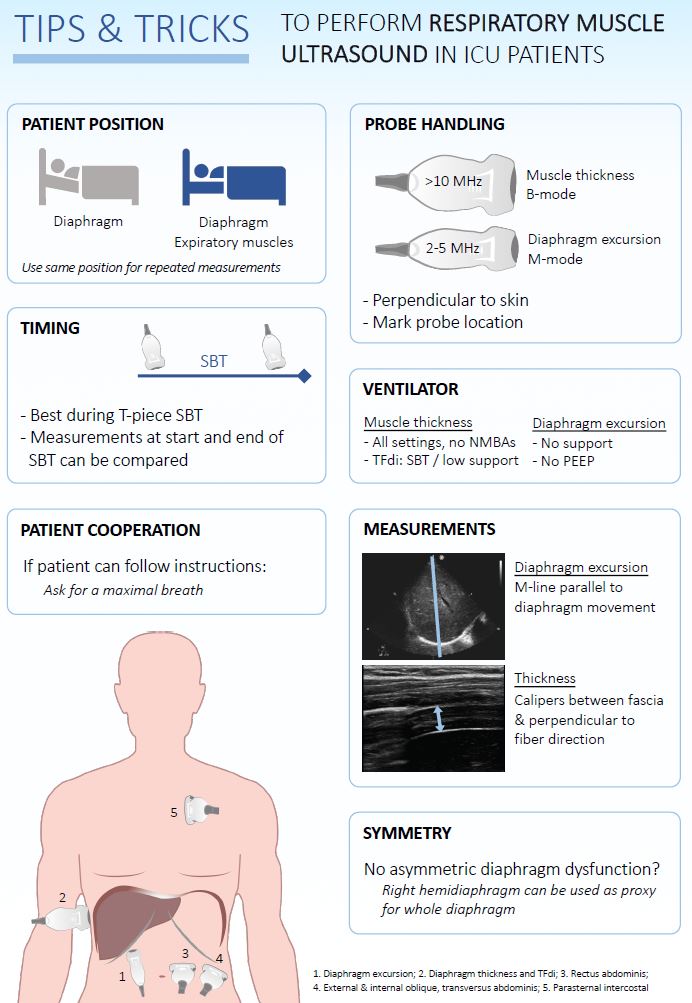
Ref: 12. Tuinman PR, et al. Respiratory muscle ultrasonography: methodology, basic and advanced principles and clinical applications in ICU and ED patients-a narrative review Intensive Care Med. 2020 Jan 14
Chief-editors
Pieter Roel Tuinman, MD, PhD, intensivist-epidemiologist
David van Westerloo, MD, PhD, intensivist
Editors:
Carlos Elzo Kraemer, MD, intensivist
Jorge Lopez Matta, MD, intensivist
Paul Wijnandts, MD, intensivist
Jasper Smit, MD, PhD student
Mark Haaksma, MD, PhD student
Micah Heldeweg, MD, PhD student
Annemijn Jonkman, technical physician, PhD student
Heder de Vries, MD, PhD student
Contact
Department of Intensive Care Medicine
Amsterdam University Medical Centres, Vrije Universiteit Amsterdam
Room ZH - 7D-166
De Boelelaan 1117
1081 HV Amsterdam, The Netherlands
prtuinman@hotmail.com
Department of Intensive Care Medicine
Leiden University Medical Center (LUMC)
